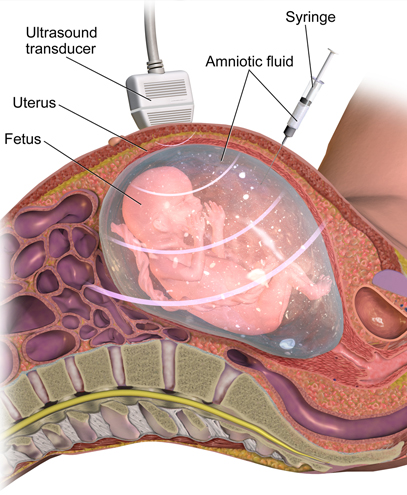
How is Amniocentesis Performed?
The procedure is usually done after the 16th week of pregnancy (second trimester), when there is enough amniotic fluid around the fetus. Here’s what happens during the test:
The pregnant mother lies on her back while the radiologist performs an ultrasound to check the baby’s position, the placenta, and the safest area to collect fluid.
Under continuous ultrasound guidance, a very thin needle is carefully inserted into the uterus through the abdomen.
Around 20 ml of amniotic fluid is withdrawn into a syringe. The procedure is done in a way that avoids contact with the fetus.
Once collected, the amniotic fluid sample is sent to the laboratory for further analysis.
The test usually takes 15–20 minutes, but the actual needle procedure may last only a few minutes. Most women can return home the same day, although doctors recommend rest for the next 24 hours.
What Tests Are Done on Amniotic Fluid?
The collected amniotic fluid is rich in fetal cells and genetic material. Depending on the suspected condition, different tests may be performed:
Karyotyping – checks the number and structure of chromosomes; helps detect conditions like Down syndrome, Turner syndrome, or Edwards syndrome.
FISH (Fluorescence In Situ Hybridization) – provides rapid results for common chromosomal abnormalities.
Microarray Analysis – provides detailed information about small chromosomal changes that may not be visible in karyotyping.
DNA testing – identifies specific single-gene disorders if there is a family history.
These tests provide crucial information for doctors and parents to make informed decisions regarding pregnancy care.
What Conditions Can Amniocentesis Detect?
Amniocentesis can help diagnose:
- Chromosomal abnormalities like Down syndrome (Trisomy 21), Edwards syndrome (Trisomy 18), and Patau syndrome (Trisomy 13).
- Genetic disorders such as thalassemia, sickle cell anemia, muscular dystrophy, and cystic fibrosis.
- Neural tube defects like spina bifida.
- Certain metabolic conditions.
- However, it is important to understand that Amniocentesis cannot detect every possible birth defect, such as heart defects or cleft lip, which are usually identified on ultrasound.
Is Amniocentesis Safe?
This is the most common concern among expectant mothers. The procedure is generally considered safe when performed by experienced specialists under ultrasound guidance. However, like any medical procedure, it carries some risks, including:
Risk of miscarriage (very low, in expert hands).
Mild abdominal cramps or spotting for a day or two.
Infection or injury to the baby (extremely rare with ultrasound guidance when done by experts).
Doctors usually recommend Amniocentesis only when the benefits of obtaining diagnostic information outweigh the small risks involved.
Role of Amniocentesis in a Healthy Pregnancy
For most women with low-risk pregnancies, Amniocentesis is not required. But in high-risk pregnancies, this test provides clarity and reassurance. It helps parents and doctors:
Confirm or rule out genetic conditions.
Plan the course of pregnancy and delivery.
Decide about special care or interventions needed after birth.
Prepare emotionally and financially for a child with special needs, if diagnosed.
In short, Amniocentesis empowers families with knowledge and helps doctors ensure the best care for both mother and baby.
Recovery after Amniocentesis
After the procedure, most women feel fine, but some may experience mild cramping. It is advised to:
Rest for the next 24 hours.
Avoid heavy lifting or strenuous activity for 2–3 days.
Contact the doctor immediately if there is heavy bleeding, severe abdominal pain, or fluid leakage.
Myths and Facts about Amniocentesis
Myth: Amniocentesis is unsafe for every pregnancy.
Fact: When done by experts, the procedure is very safe and complications are rare.
Myth: It is painful.
Fact: The procedure may cause mild discomfort, but it is not extremely painful. Local anesthesia may be given in some cases.
Myth: It is only done in abnormal pregnancies.
Fact: It is mainly recommended when risks are high, but in some families with a history of genetic disorders, it may be planned even in a normal pregnancy.
When it plays a key role
You should discuss with doctor if:
You are over 35 years of age.
Your screening test or ultrasound shows abnormal results.
You or your partner have a family history of genetic disorders.
You had a previous child with genetic abnormalities.
Your doctor will guide you on whether the test is necessary in your case.